One 10cm plate and seven screws later.
TL;DR: sleep is important
I broke my jaw at the end of August by standing up and fainting—way to go, right? I got up out of bed in the morning, felt dizzy, blacked out, and fell. I woke up within a few seconds and noticed that my jaw felt out of place. The left side felt stuck higher up, so the right side of my bite didn’t close. I also had a scrape on my chin and my ear was bleeding.
My mom rushed me to the dentist, where they did a panoramic dental x-ray to find that my jaw was fractured in two places.
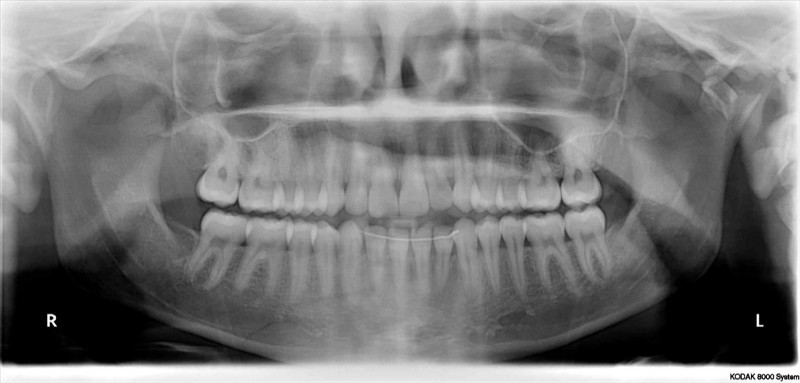 The original panoramic x-ray result. The white line across my lower middle
teeth is my permanent retainer!
The original panoramic x-ray result. The white line across my lower middle
teeth is my permanent retainer!
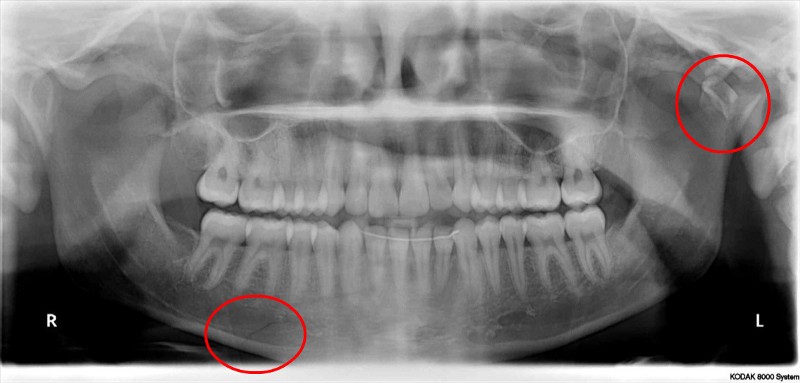 The two fractures: the body fracture on my right and the condylar fracture high
up on my left.
The two fractures: the body fracture on my right and the condylar fracture high
up on my left.
The doctors identified two fractures: one along the body of my jaw and one high up on the left condyle [diagram] and recommended I go to the hospital for surgery. This blog post recounts my experiences from injury to full recovery, and is basically everything I wish I’d known before it happened.
- The Hospital
- The Surgery
- Immediately Post-Op
- 1 Day Post-Op
- 2-3 Days Post-Op
- 4 Days Post-Op
- Week 1
- Week 2
- Weeks 3 + 4
- Weeks 5 + 6
- Arch Bar Removal
- Weeks 7+
- Why did I fall?
The Hospital
After I was admitted to the hospital I waited and napped for a long time. It was overall fine and relaxing, but my IV for fluids was annoying to move around with. Throughout the day I met with various doctors and nurses: oral & maxillofacial surgeons for the surgery, and internal medicine doctors to investigate why I fell.
I could talk alright before the surgery, but couldn’t open my mouth very much, chew, or brush my teeth. I never felt much pain while waiting — I didn’t really feel the fracture along the body at all, and the condylar fracture only hurt when I tried to open my jaw wide. The doctors and nurses were very concerned about my ear bleeding, but that turned out to just be a surface cut. I had a CT scan at the hospital to better understand the injury and decide which surgery to do.
The Surgery
For the fracture on the jaw body, the doctors decided to do an “internal fixation”, where they put a small titanium plate across the break to fixate it. The plate looks like this:
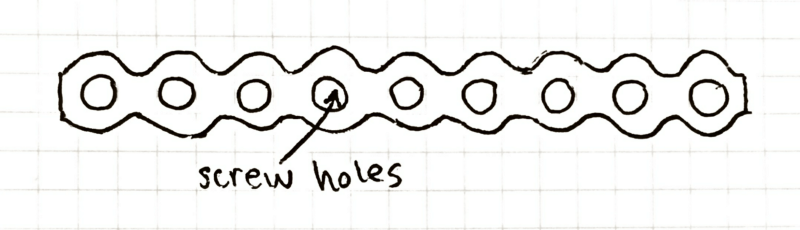
The plate goes from a bit before the corner of my jaw on the right to a little past the curve at the front of my chin. The plate is 10cm long (about the length of my index finger), 1.7mm thick, and held on by 7 titanium screws. The plate had to be so long because the fracture was sort of parallel along the bone. It’s made to stay in for life.
With the condylar fracture, the head of the condyle actually broke off of the bone and is “floating” in that area. Because it’s so high up in the joint, the surgeons decided not to open up the joint area and fixate it with a plate — it’s an invasive surgery and could have caused problems with articulating my jaw. Instead, they decided to temporarily lock my jaw shut with arch bars and elastic bands.
 Arch bars (image source)
Arch bars (image source)
Arch bars are like a row of braces above your teeth with little metal hooks like a coat rack for hooking the elastics. The bars are held on by wire twist-ties “lassoed” around each tooth. They decided to use elastic bands instead of wires because my jaw could have locked if the condyle healed without any movement. The elastics were moved and adjusted as I healed, allowing for more and more guided movement.
To put in the plate, the surgeons made an incision inside my lip (like if you pulled down your lower lip all the way, and cut at the line between lip and gum). They stitched it up with dissolvable sutures.
For the surgery itself, I changed into a hospital gown and socks, peed extensively so I wouldn’t need to during surgery, and talked with the main oral surgeon and anesthesiologist. They gave me the KO medication through my IV and I was completely out for the 3–3.5hr surgery.
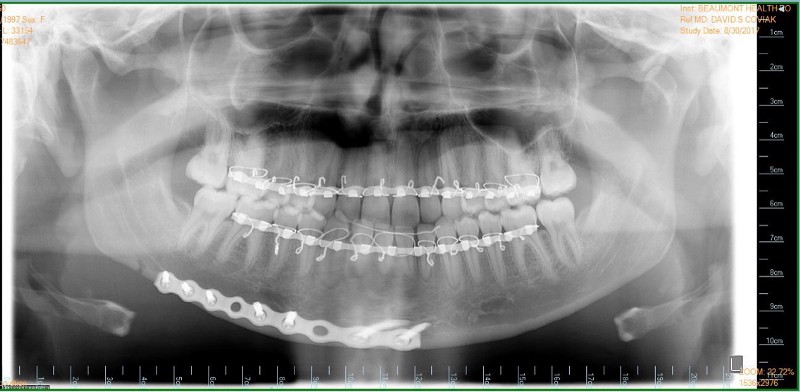 The plate and arch bars after the surgery (same as first image).
The plate and arch bars after the surgery (same as first image).
Immediately Post-Op
I was SUPER PUFFY and could not feel most of my lower lip and jaw area, but still wasn’t really in any pain. I couldn’t move my jaw or open my mouth to speak. My throat was a bit scratchy because they had to put a tube up my nose and down my throat for anesthesia. I drank chicken broth and rested for the rest of that day and night.
1 Day Post-Op
I was still just as puffy the day after the surgery. I kept drinking water and broth and getting IV fluids. I also showered, which was a bit scary because I was afraid of falling again (except naked this time), but it went OK. I used Vaseline to keep my lips from getting chapped for the next month, because I couldn’t open my mouth to lick my lips.
I was given 5 medications:
- Antibiotic (amoxicillin) every 8hrs for a week. Sweet pink liquid.
- Prescription painkiller (hydrocodone) as needed. I only took this once, and just used ibuprofen from then on, because I wanted to avoid opioids.
- Non-prescription painkiller (children’s ibuprofen) as needed. I took this every 8hrs with my antibiotic. White/clearish and sweet, but stung my throat a bit.
- Strong mouthwash (chlorohexidine) rinse after every meal because I couldn’t open my mouth to brush my teeth. Medical-grade alcohol-free mouthwash.
- Anti-nausea and anti-constipation meds to combat possible side effects from the hydrocodone. I never used these.
At the end of the day I finally had my IV taken out and went home!
2-3 Days Post-Op
For the next few days I just took medicine and rested. I used a bed wedge at home to rest with my head elevated and ordered one for school too. I could only drink extremely smooth things because I could only sip through the space between my upper and lower teeth. Example liquids:
- Juice
- Cream of {Chicken, Mushroom, etc.} soups (strained)
- Broths
- Ensure/Premier Protein
- Smoothies (strained only, but this was still very difficult and didn’t really work)
I flew to Boston for my fall semester of school 3 days after my surgery. The flight was uneventful — the TSA inspected my ice packs, but I was convincing enough that I needed them (I was puffy as heck, couldn’t speak, and had a plastic bag full of medicine!).
4 Days Post-Op
I was fortunate to be able to stay with my boyfriend’s family in the Boston area for a day before moving back into my dorm. At first I used a text-to-speech app to talk, but then I started to become able to speak in a garbled voice without moving my jaw or lips much.
I had a lot of angst over meeting my boyfriend and his family because I was really embarrassed with how I looked. He, his family, and all my friends were really kind and supportive, though, and it meant a lot to me.
I was still very puffy, but my chin scab started to heal. The skin on my face peeled a little (making room for puffier skin), and so did the skin on my lips. My mouth felt fuzzy and gross from not brushing… pretty much from then until I could brush my teeth again.
Week 1
It was very difficult to talk. My mouth had a bit of a lingering taste of blood, and my spit was always red/pink. Keeping up with antibiotics and pain meds every 8 hours was annoying, but I’m glad I was never really in pain.
Once I was in Boston, I made weekly appointments with Dr. Somi Kim at Massachusetts General Hospital (MGH). Dr. Kim was really nice! She adjusted the locations of my elastics so that my bite was back to where it naturally rests, which was a huge relief. It had been a bit out of place since the surgery, with my bottom front teeth pushing on my top front teeth. She also told me not to do any contact sports for 3 months, and that I was absolutely not allowed to chew for the next 6 weeks.
The most surprising thing she said was that it’s possible to remove the plate! I had expected to have to keep it in forever, but it can be removed after 6 months. It’s still worth a discussion whether the removal is worth it.
As far as swelling, Dr. Kim said that 50% of the swelling goes down in the first 6 weeks, and the next 50% goes away in the next year. For me most of the swelling went away after 2.5 weeks, though.
 Me (left) struggling to smile normally at HackMIT 2017 (2.5 weeks
post-op). You can see my arch bars peeking out, and my right side is still a
little puffy.
Me (left) struggling to smile normally at HackMIT 2017 (2.5 weeks
post-op). You can see my arch bars peeking out, and my right side is still a
little puffy.
My lower right lip and cheek near the plate were numb for a long time after surgery because the nerve that passes through that area was skeletonized. I was still pretty numb even after the swelling went away. At 3 months post-op I had about 90% of the feeling back, and at 4 months now I have 95%+ back, but I was worried at the beginning because the numbness receded so slowly.
Week 2
During week 2 talking got easier, but I still couldn’t move my jaw at all. The bruising/swelling started turning yellow. One of my elastics broke at this time, and I was TERRIFIED of putting it back in. I was afraid of tearing my stitches, and didn’t know exactly which hooks the elastic was supposed to go on. It took me like 30 minutes and I almost cried from stress. I got way better at putting these back on by the end.
At this week’s doctor’s appointment I was put in lighter “guided elastics” that let me open my mouth. I had an elastic band on each side of my mouth in the following positions:
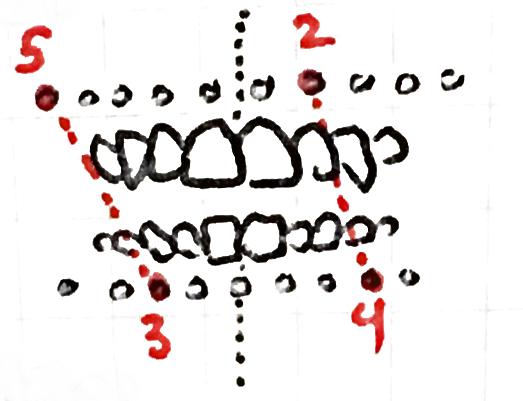 I remembered the positions as 5–2–3–4, like room 5-234 for HackMIT meetings!
I remembered the positions as 5–2–3–4, like room 5-234 for HackMIT meetings!
I had to take the elastics out 3 times a day and stretch open my jaws as far as I could. This sounded scary based on my last elastic replacement experience, but it was way easier when my stitches were healed (at around 3.5 weeks in!). I didn’t really get around to doing the jaw exercises 3 times a day, but I did do 2 times (morning and night). I also stopped taking ibuprofen for pain around this time.
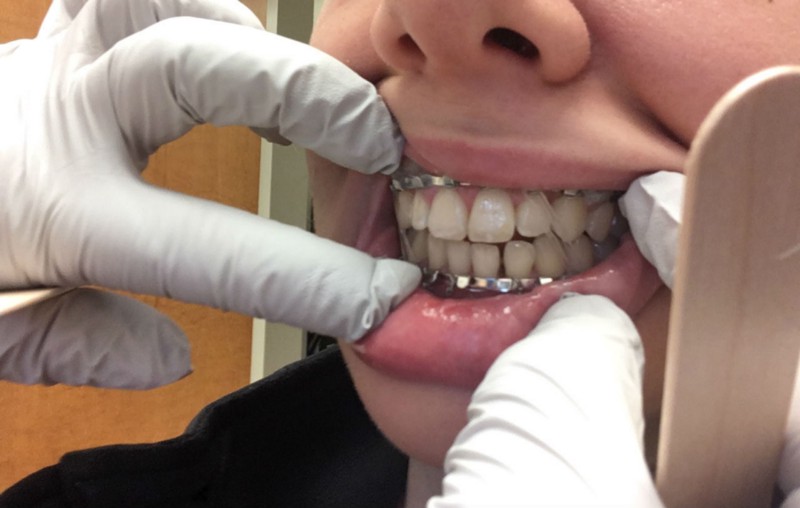 Guiding elastics in my mouth IRL.
Guiding elastics in my mouth IRL.
Other miscellaneous notes:
- Using a waterpik would have been fine as long as I didn’t blast my stitches. I was ultimately too afraid of this to use it, though.
- Sleeping on my side was fine as long as it didn’t hurt (ordering a bed wedge was a bit of overkill I guess, haha). I was very concerned about my bite alignment slipping out of place when I relaxed, but Dr. Kim reassured me it would go back to normal (and it did). The condyle on the left side is slowly regrowing to match the right, so over time it’s becoming more and more even.
- I read online that chlorohexidine (the strong mouthwash) could stain your teeth, but Dr. Kim reassured me that a regular cleaning at the dentist’s would fix it. I didn’t end up having noticeable stains. I switched to a regular alcohol-free mouthwash when I ran out of chlorohexidine.
I only had trouble sleeping for one night in the whole recovery period, 13 days post-op. For some reason my jaw just hurt a lot being in the aligned position, but I was afraid to let it rest in the askew position while I slept in case it stayed there. I just took some ibuprofen and stressed myself out until I fell asleep at 4am. My worry ended up being unfounded — my bite got more and more even, and I had a comfortable and fairly even bite by week 4.
Weeks 3 + 4
By week 3 I looked pretty much normal and got a lot better at speaking without moving my jaw. I spoke on the mic in the arena at HackMIT without sounding very distorted, and I didn’t need to preface conversations with new people by explaining that I broke my jaw. I just looked like a slightly less symmetric version of myself with weird braces.
Having room to open my mouth also made eating so much easier! My eating pattern was to take miscellaneous smoothie ingredients in a green box from the dining hall up to my wing’s main lounge, blend them, and supplement the mix with Ensure or Premier Protein. I got tired of Ensure’s distinct flavor (vanilla tootsie rolls) and started drinking Soylent, which I liked a lot.
Throughout all of this, eating took much, much longer than usual. Drinking food instead of chewing it probably takes twice as long.
Another breakthrough I had during this time was to use orthodontic wax! Before I used it I couldn’t really laugh or smile without being lacerated with all the wires. The wax made my mouth bulkier, but was definitely worth it.
Maybe my favorite milestone of week 4 was being able to take out my elastics and
brush all of my teeth with a manual toothbrush!! ![]()
![]() It felt SO
GOOD.
It felt SO
GOOD.
Weeks 5 + 6
I only had to wear my elastics at night for these last 2 weeks. I was told to do jaw exercises more frequently (5x/day for 5min each), but I didn’t remember this very well and just tried to practice whenever I remembered.
It was a bit tough to remember not to chew while my mouth was totally free, but I stuck with it. I could mush things in my mouth like oatmeal, cream of wheat, chili, soup, cottage cheese, soft pasta, and scrambled eggs. I got pretty good at swallowing small soup ingredients like kidney beans or chickpeas without chewing them. Instead of going up to the main lounge and blending things, I would drink cups of soup and milkshakes in the dining hall.
I started using my electric toothbrush and flossing too, which felt amazing
![]()
Arch Bar Removal
I was so excited to have the arch bars gone!! There were 3 possible anesthesia methods to remove my arch bars:
- Swish lidocaine in my mouth: tastes bad, but it’s easy. Maybe not as numbing as the other options.
- General anesthetic: going totally under. It’s kind of a big deal and takes a lot of time for how short the operation is.
- Injections: I’d need 7–8 shots to numb enough of the lip area, so it’s almost as much work and pain as the removal itself.
I decided to go with the lidocaine. I was worried because Dr. Kim said it was “uncomfortable”, but it was really fine. It took about 10 minutes, and felt like… getting wires pulled out from between your teeth, which is what it was. She untwisted the wires, snipped them short, then pulled them around and out. I grimaced for a few of the pulls, but it was fairly quick and I really wanted it all gone.
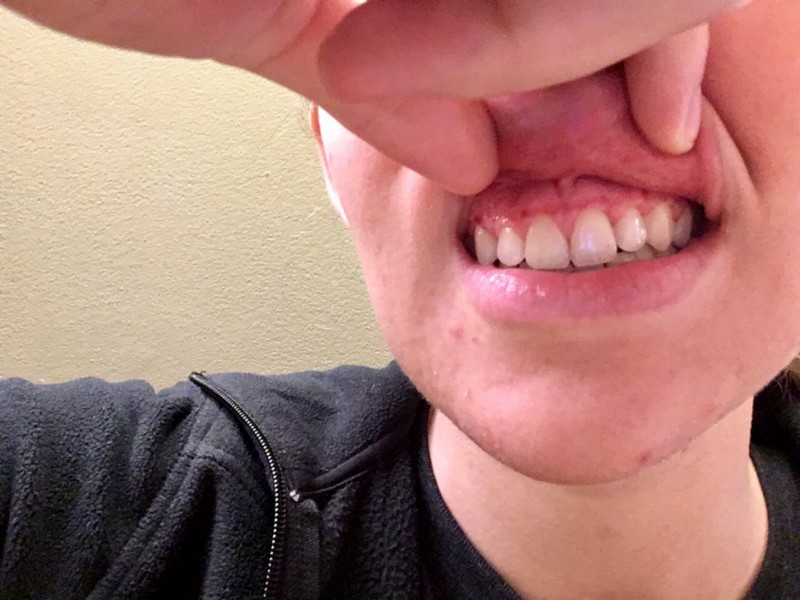 Imprint of the removed arch bar!
Imprint of the removed arch bar!
Weeks 7+
My first meal after I could chew was a super lame sandwich. ![]() Chewing felt weird, but good. Putting my clear retainer back on my top teeth
hurt really bad at first, but it did fit and went back to normal.
Chewing felt weird, but good. Putting my clear retainer back on my top teeth
hurt really bad at first, but it did fit and went back to normal.
Food gets stuck in the lower right side of my mouth sometimes, probably because the stitches made the pocket a bit smaller. It’s a bit annoying but I think it’s getting better, or I’m getting used to it. I had to work up to chewing really crunchy things, but it only took maybe a week.
At my last dentist appointment everything checked out, and I feel 100% normal
now ![]()
Why did I fall?
Tests in the hospital ruled out any serious brain or heart issues. I still feel faint sometimes when standing up quickly, but I’m careful now to wait a bit before getting up, or I just sit down on the floor carefully as I start to feel it. I feel more dizzy when I’m sleep deprived, so I think I fainted because I went to bed too late the night before I fell. Let this be a warning that getting good sleep is extremely important, and lack of sleep can have drastic effects on your health and body! I’m still learning this, and feeling the plate under my skin is a firm reminder to keep improving and building good habits.
I’m very thankful to Dr. McLean at the dentist’s office for taking my x-ray on such short notice, Dr. Pokorney and the Beaumont OMFS staff for doing my surgery so well, Dr. Kim at MGH for being so patient with all my followup questions, my boyfriend and his family for hosting me in Boston while I recovered, my friends for all being so accommodating and understanding, and of course my family for helping me through everything and keeping me company in the hospital.
When I first got hurt, I worried a lot about what was going to happen and if I was ever going to be okay again. Reading about other people’s experiences helped me get a feel for what I should expect, so I hope that someone can benefit from reading about my experience.
Thanks to Noah Moroze and Kimberli Zhong for feedback. This blog post was cross-posted on Medium here.